Minimally Invasive Sacroiliac Joint Fusion
Sacroiliac joint dysfunction is a common cause of back pain. Sacroiliac joint pain(SIJ pain) can mimic discogenic or radicular low back pain. Patients with SIJ pain often report low back, groin, and/or buttock pain. 15-30% of all cases of low back pain are thought to originate from the sacroiliac joint. It is also thought that up to 75% of lumbar fusion patients will develop significant sacroiliac joint degeneration after 5 years. While sacroiliac joint injections and physical therapy sometimes provide long term benefit, often the relief from these interventions is short term. Traditional open joint surgeries require large incisions, significant bone harvesting, significant hospital stays and long recovery times. There are now minimally invasive options to provide long term benefit from sacroiliac joint dysfunction.
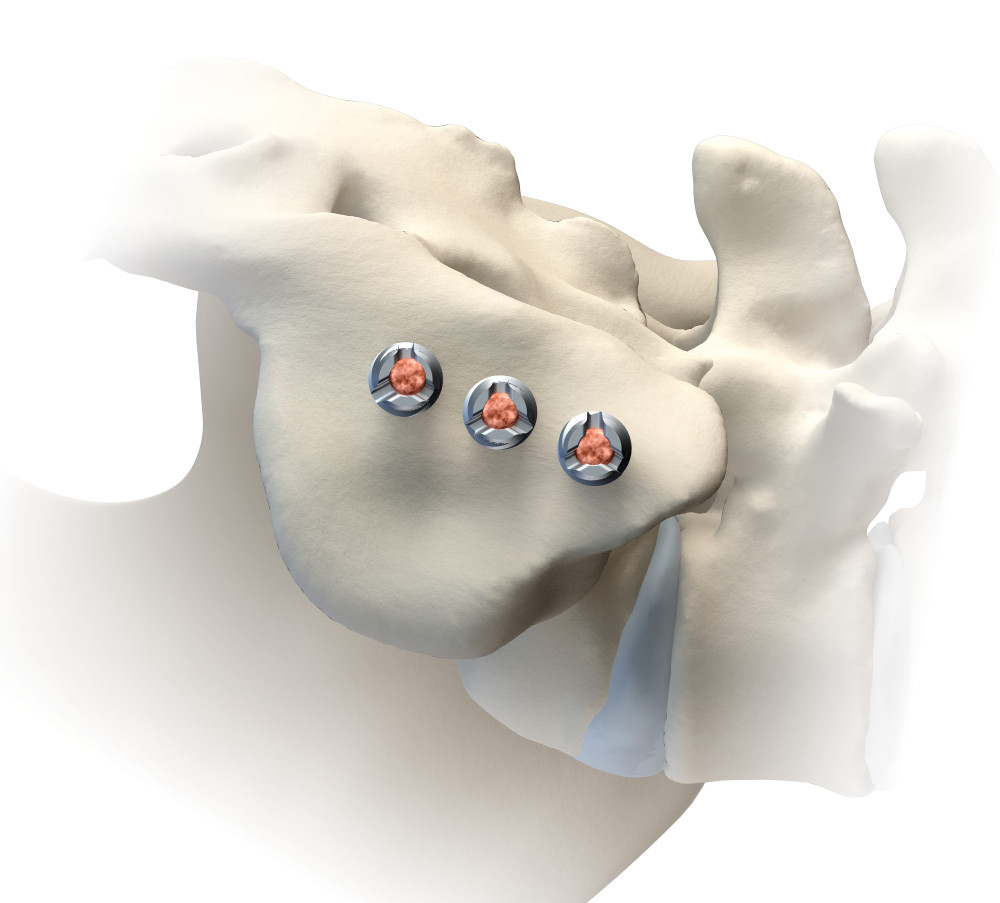
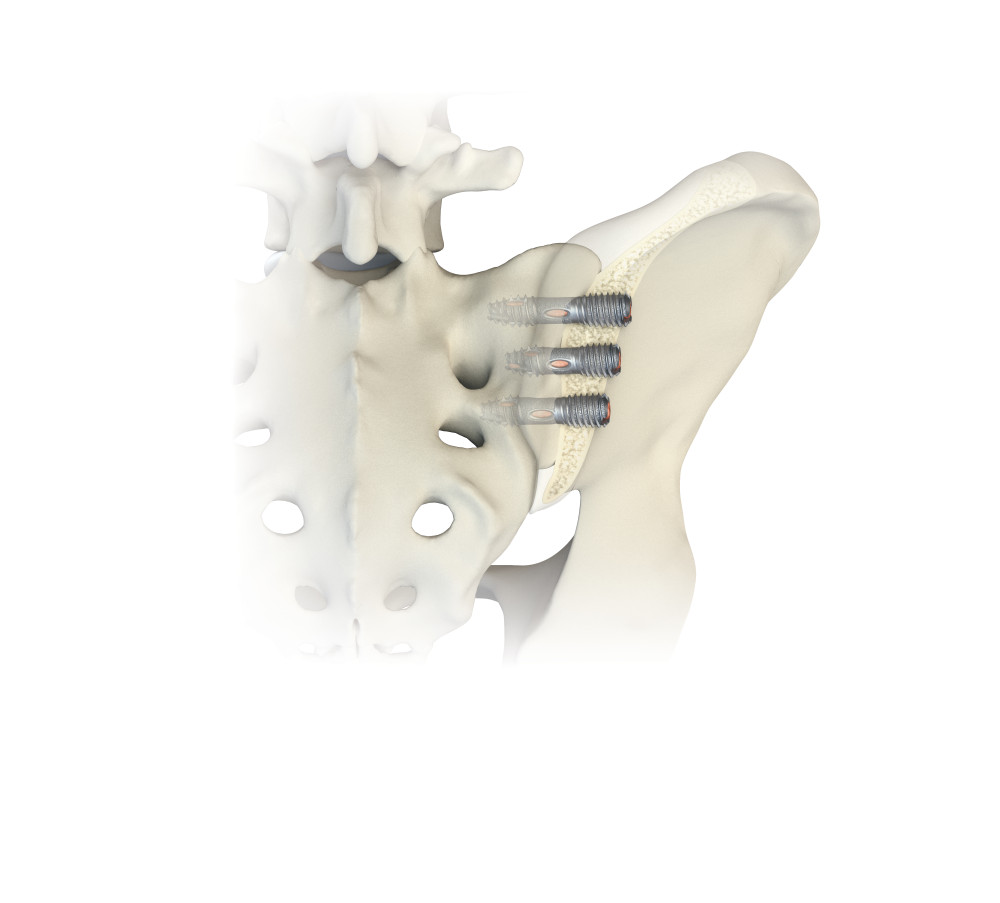
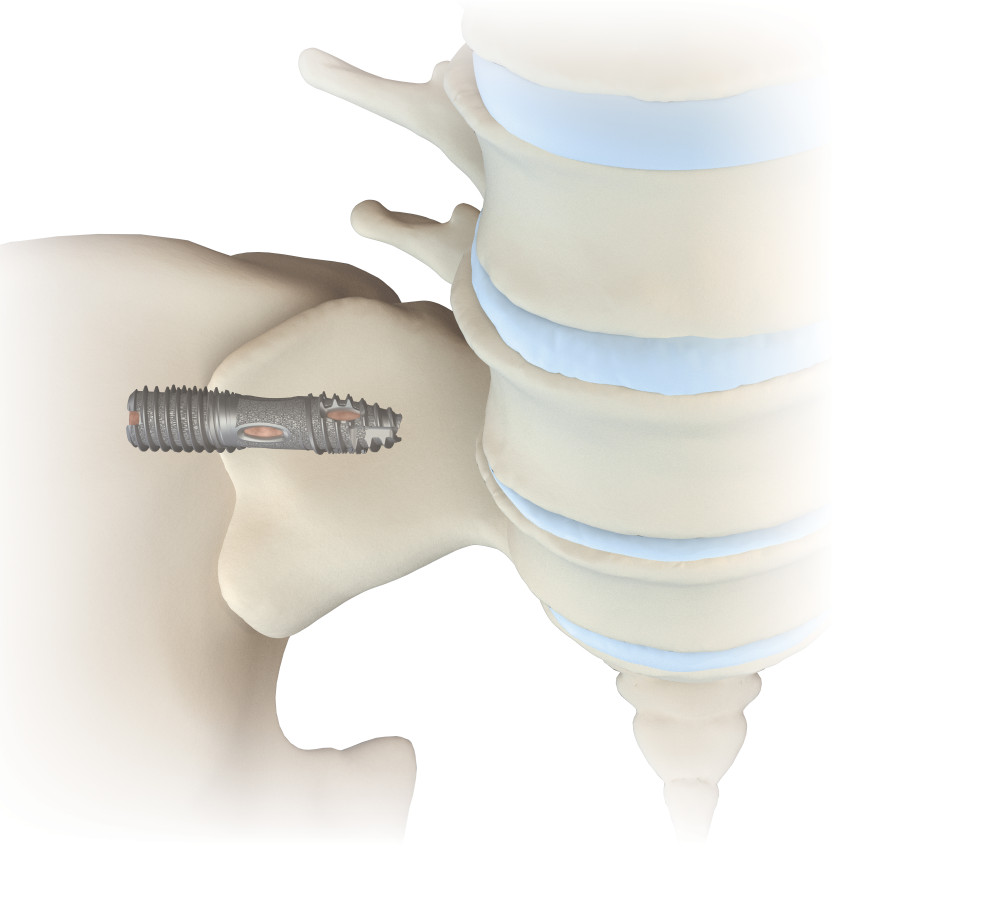
Lateral approach
This is a minimally invasive approach that places two to three small screws across the sacroiliac joint. While this procedure is slightly more invasive, it likely allows for quicker stabilization, as the screws will immediately stabilize the joint. The screws are specially designed to allow controlled compression across the joint as well as to minimize migration. The procedure is performed through a small incision. The procedure is typically performed in less than one hour, as an outpatient, with minimal blood loss and quick recovery. The procedure can be performed with moderate to deep sedation and does not always require general anesthesia.